Questions and Answers
Consultation
Snoring
Many symptoms can be experienced by a person with sleep apnea. The most common are:
- Sore throat and dry mouth upon awakening
- Snoring
- Choking sensation at night
- Daytime fatigue and lack of energy
- Fatigue when driving
- Headaches in the morning
- Poor sleep
- Memory disorders and mood changes
- Libido decline
- Frequent waking during night and insomnia
However, it is common that a patient with sleep apnea does not suspect it by himself. It is often the life partner who informs the patient that he snores and stops breathing momentarily during sleep.
The best indicator for the patient is definitely non-restorative sleep and daytime sleepiness. This is why screening for sleep apnea is frequently done using a questionnaire called the Epworth sleepiness scale.
If you have reason to believe that you suffer from sleep apnea, it is important to consult a sleep professional for a complete sleep evaluation. A sleep study at home or in the laboratory is the only way to diagnose apnea and to evaluate its severity.
The answer to this question is yes! There are many solutions for a snoring problem and several of them are very effective.
Recognizing the snoring problem is the first step towards solving it. The next step is to consult a sleep specialist or a health professional that can assess your problem. Snoring can be a sleep apnea symptom which has adverse health consequences over time.
You will find many gadgets on the web that promise to solve your snoring problem. You should know that the effectiveness of these devices is often limited, plus they can sometimes cause damage to the teeth, oral tissues and nasal passages. However, the main problem of these non-prescribed devices is that they can hide a potential sleep apnea problem. It is essential to examine any snoring problem by consulting a professional to rule out sleep apnea that would require a different treatment.
Solutions and advice on healthy lifestyle will be proposed once the snoring diagnosis is established. The mandibular advancement device (MAD) and the uvulopalatoplasty by radiofrequency are the most commonly recommended treatments to our patients. The MAD is particularly effective in patients who snore or have sleep apnea when lying on their back, which is a factor that may aggravate the problem, when compared to sleeping on your side or on your stomach.
During your consultation in a snoring and sleep apnea clinic, the specialist will present you the options that may work well for you. Snoring can be treated effectively. There is no reason to endure it any longer.
Snoring can affect both your spouse’s sleep quality and your own. Loud snoring can compromise a couple’s relationship and may sometimes require partners to sleep in separate rooms. This can affect a couple’s intimacy and therefore progressively set lovers apart.
There are several good reasons to treat snoring. These include good quality sleep and health problems prevention. Maintaining a harmonious relationship is an equally important reason, as it can improve a patient’s mental health and well-being.
Sometimes snoring can be a source of conflict and frustration in a relationship. The person who is sleep deprived by the partner’s snoring is frustrated and the snorer feels guilty, ashamed, and helpless. These feelings may set apart even the closest of couples.
Although some couples do not feel affected by sleeping in separate rooms, most people will prefer to find a solution in order to sleep together again. In fact, most couples will see a decrease in physical contact over time when forced to sleep in separate rooms because of their partner’s snoring. This lack of physical proximity will inevitably affect the couple’s emotional connection.
Several treatments are now available to treat snoring. A consultation in a specialized clinic followed by a sleep study will help determine the exact cause of snoring and establish an appropriate treatment plan. The costs of these treatments are affordable but not covered by private insurance or Medicare when it comes to simple snoring without sleep apnea. Most treatments are very well tolerated and recovery is rapid with little pain. The evaluation, the treatment plan and the execution of it may take a total of six to eight weeks at our clinic.
This situation is very common. A lot of patients with snoring problems consult because a relative has made an appointment for them. Of course, you cannot force your spouse to seek treatment, but you can explain to him your concerns for his health. Explain to him the facts about the risks of sleep apnea: increased risk of heart attack, high blood pressure, arrhythmia, etc.
Having a life partner who snores can be very frustrating. Studies show that a person sleeping next to a snorer loses an average of one hour of sleep per night. If your partner is not concerned with his own well-being, he should be for yours. Snoring has an impact on you and possibly on your relationship. Some partners realize the extent of the problem when their spouse begins to sleep in a separate room. Let him know that his behaviour affects those around him.
Finally, some people refuse to face reality. Perhaps because they are ashamed, they refuse to admit that they snore or they stop breathing. In these cases, recording your partner’s snoring is a solution that usually works well.
How are snoring or apnea treating devices made?
Are chin straps an effective snoring treatment?
I saw a device on the Internet against snoring. Is it effective?
The device for snoring is called mandibular advancement device (MAD). Its conception is a painless process and requires no anesthesia. The first step in making such a device, either to counter snoring or apnea, is a full clinical mouth examination.
A panoramic radiograph and a 3D scan of your mouth and your temporomandibular joints are required. The purpose of this evaluation is to determine if you can benefit from a MAD safely. The professional must ensure that your teeth are strong enough to bear the device. The jaw joints should also be healthy.
If the specialist determines that the MAD is for you,a second appointment is booked to take impressions of your teeth. Using a special paste, your upper and lower teeth are registered to make an exact replica of your mouth. The specialist then records your occlusion so that the device is crafted in the right position. The models of your mouth will be sent to the laboratory with detailed instructions ensuring the device is manufactured according to the treatment plan. This usually requires a period of 2 to 3 weeks.
At your third appointment, the specialist will make the final adjustments to optimize efficiency and comfort. Advice will be provided verbally and in writing in order to facilitate device wear and keep it in good condition as long as possible. Follow-up visits are to ensure the proper function of the MAD and to make corrections if necessary. The frequency of these visits will be determined depending on the patient’s condition and clinical situation.
Are chin straps an effective snoring treatment?
Most patients who shared their experiences regarding the chin bandages purchased them over the Internet. Unfortunately, mainstream media frequently report incomplete or incorrect scientific results. This may mislead patients about the real impacts of a given treatment. Studies of companies offering various products to treat snoring and apnea are often misleading and findings are used to promote their products.
The chin straps are often used with a positive pressure (CPAP) therapy to prevent the pressurized air from escaping through the open mouth. However, their exclusive use brings few benefits. Although some studies have demonstrated the effectiveness of chin straps in the treatment of sleep apnea, the reported cases are anecdotal and the vast majority of patients will see no improvement in their sleep apnea and / or snoring when using these straps.
A study by the Journal of Clinical Sleep Medicine, a journal whose articles are reviewed by sleep experts before publication, reported in August 2014 having studied the cases of 26 patients with obstructive sleep apnea for which a treatment with a chin strap was done. Among these patients, none showed apnea or snoring improvement, which seems to confirm the limited effectiveness of this therapy.
Patients with mouth breathing and simple snoring could theoretically benefit from these devices. But most people who breath through their mouth at night, do so because of difficulty breathing through the nose. It would be more appropriate for these patients to first treat their nasal obstruction problem in order to obtain definitive symptom relief. The chin straps do not seem to be an effective treatment and should not be considered.
A reliability problem
The internet is full of websites selling different products to counter snoring. The main attractions these websites put forward are that devices are inexpensive and there is no need to consult a professional in order to get them. Everything is presented in a tempting way and the offer seems too good to be true.
What seems too good can actually hide the truth. Most media who sell these devices are not linked to any professional order and profit is often their main priority. Some scientific facts reported are incomplete or simply wrong. The studies presented are often carried out by the group that sells the device in question and the results are usually biased in favour of the product.
A sleep professional is a person who studied in the medical field. One of the fundamental principles of modern medicine is the so-called “evidence-based practice”. For any treatment offered in our clinic, we will be happy to answer your questions and introduce you to the independent literature that justifies its use. Our professionals are also bound by the ethical codes of their professional orders, to which you can have recourse in case of litigation. It is difficult to say the same for most web sellers.
Snoring is probably not just simply snoring
In our opinion, the main problem devices sold on the Internet present is self-diagnosis. If you buy a device in order to solve your snoring problem, this may hide underlying sleep apnea. This is a serious condition that can have important consequences on your health. A professional evaluation with a sleep study is ESSENTIAL if you have any doubt about your condition. To help you decide whether you should be evaluated, we suggest you do our online test.
Buying on the Internet
Once the diagnosis of only snoring is confirmed, your sleep professional can offer you solutions. You could still decide to invest in a product offered online and possibly benefit form its use. If it does not turn out to be effective, you will not put your health at stake, because only having a snoring problem has no impact on the physical health of the individual who snores.
Some devices purchased on the Internet can cause tooth movement because most are not personalized to your own teeth and no professional follow-up is done. Make sure you have a regular follow-up with a dentist because the tooth movement is irreversible (except by orthodontic treatment) and can lead to the loss of one or more teeth if too pronounced.
Sleep apnea
Sleep apnea can affect patients of all ages and even children. Risk factors for sleep apnea include the following:
Obesity
Excess weight is a contributing risk factor for sleep apnea. The fat is deposited around the upper airways, which gradually reduces their diameter.
Male gender
Men are 2 times more likely to suffer from sleep apnea. However, the difference in risk is diminished when a woman is overweight or reaches menopause.
Age
Patients older than 40 are more likely to develop sleep apnea than younger patients. The risk increases significantly after the age of 60.
Neck circumference
An increased neck circumference (17 inches or more in men and 16 inches or more in women) is a risk factor, as the size of the airway is reduced.
Unfavorable anatomy
Some people are born with hypertrophic tonsils, large tongues, or retrusif jaws. This can contribute to airway obstruction and promote apnea.
Genetics
You will have a greater chance of developing sleep apnea if one of your family members suffers from it.
Smoking
Tobacco use increases airway inflammation and promotes water retention. The risk for smokers is estimated to be 3 times higher than non-smokers.
Nasal congestion
Nasal obstruction caused by a deviated septum, allergies or sinus problems can affect nasal breathing and thus increases the risk of sleep apnea.
Alcohol, sedatives or tranquilizers use
These substances cause throat muscles relaxation, therefore decreasing air passage.
A CPAP machine will essentially push air down your throat so that it does not close. This will avoid the “choking” or sudden awakening that happens during sleep. The symptoms are less tiredness, less risk of hypertension and other benefits associated with getting a good night sleep.
I have sleep apnea. Is it dangerous for me if I get the Coronavirus?
The American Academy of Sleep Medicine did write an article about Coronavirus FAQs: CPAP tips for sleep apnea patients. Here is the link of the article : https://aasm.org/coronavirus-covid-19-faqs-cpap-sleep-apnea-patients/
Can children have sleep apnea?
Sleep apnea can affect individuals of any age. Children are therefore unfortunately not spared from this condition. Here are the symptoms that you should look out for:
- Your child snores loudly. This can be accompanied by sounds of gasping or grunting.
- Your child’s breathing temporarily stops for longer than two inspiration / expiration cycles.
- Sweating at night due to the increased breathing effort.
- Your child wakes up with a headache. He shows daytime sleepiness, irritability, hyperactivity or difficulty concentrating.
Apnea in children has characteristics that are slightly different from adults. The diagnostic criteria are somewhat stricter regarding AHI in children. Causes can also be a little different than those for adults. Naturally small airways children can make air passage difficult. With growth, it is possible that the problem disappears. Tonsils and adenoids are frequently the cause of snoring and apnea in children. Surgery can therefore solve the problem for most young patients. If that does not work, CPAP therapy may be considered.
Just like adults, be aware that an obesity problem increases the child’s risk of suffering from sleep apnea. A healthy lifestyle is necessary. We invite you to look at our page 10 tips to reduce snoring for more information.
There are very few studies that have been done to determine the link between caffeine and obstructive sleep apnea syndrome. Among those published, the results are contradictory. One of the studies seemed to show a link between caffeinated soft drinks and an increase in apnea severity. However, the same study could not link coffee or tea with apnea. It is therefore difficult to conclude that caffeine is directly responsible.
You should also know that caffeine is used in neonatology departments to prevent apnea episodes in premature babies. Doctors prescribe the drug to stimulate the child so that he does not stop breathing during sleep.
For now, it is not scientifically possible to conclude the link between caffeine and sleep apnea.
The fact that your husband has stopped drinking soft drinks is a positive change that may have influenced his body weight. Losing weight is a major factor influencing the severity of sleep apnea.
For more tips on healthy habits that reduce snoring, read our article about this subject.
We understand your interest in this new apnea treatment because it is a very promising one. This treatment by electrical stimulation is currently not approved by Health Canada. This treatment, marketed under the name of Inspire ®, has however been approved by the Food and Drug Administration in April 2014, which is usually a contributing acceptance factor of the treatment by Canadian authorities. It is unfortunately not possible to accurately estimate when it will be available in Canada.
This treatment involves implanting a small device that causes electrical stimulation to the hypoglossal nerve that controls the pharyngeal muscles. This stimulation is strong enough to restore muscle tone and open the airway without waking up the patient.
Sleep Study
Two types of sleep study are possible. The first type of sleep study will take place in the comfort of your home. These are the most widespread studies because they have the advantage of placing the patient in their natural environment. The second type of sleep study will take place in a sleep laboratory or hospital. A room will then be assigned to a technician.
Home sleep studies
If the sleep study that is recommended to you takes place at home, you will meet with a respiratory therapist who will explain in detail how the recording device works. He will tell you how to install the various monitors. Do not hesitate to ask questions if you have doubts about how to proceed.
Laboratory sleep studies
In the sleep lab, the electrodes that record your sleep parameters are installed by the technician. This test is more complete than a home study, as laboratory analysis also measures brain activity during sleep. Once the preparation completed, you will be asked to go to sleep.
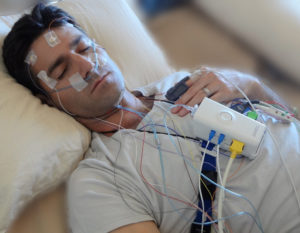
As seen above, the number of recorded parameters varies depending on the type of sleep study. According to the American Academy of Sleep Medicine (AASM), the sleep study should test and record a minimum of 2 respiratory parameters, cardiac activity and the blood oxygen level. To achieve this, a band is placed around your chest to measure the movements of your rib cage during breathing and a pulse oximeter will be on the tip of your finger.
In a sleep laboratory study, surface electrodes are put on your face and scalp to record electrical activity of your facial muscles and your brain. The various monitors used are:
EEG: electroencephalography to measure brain activity
EMG: electromyogram records the activity of facial and legs muscles and allows to identify the deep sleep phase (REM). It is during this sleep phase that we dream and brain activity is increased.
EOG: Electro-occulogram to record eye movements. These movements are important to identify the different sleep stages and REM sleep.
ECG: electrocardiogram to record cardiac frequency and pulse
Nasal air flow sensor
Microphone to record snoring
The monitors that will be installed will seem uncomfortable, but most patients fall asleep without difficulty whatsoever whether examinations are done in the laboratory or at home. The results will be analyzed by your healthcare professional and he will then contact you to give you the results.
The test costs $500.
For the setup, we email you with an explainer video. The setup is relatively simple, a belt to be installed at chest level, a nasal cannula and a finger saturometry. When you receive the device, you can take a look at it and contact us if you have any questions. A respiratory therapist will be able to answer them.
Yes, we do. We offer both sleep studies at home and in our lab in Montreal.
An in lab sleep test is a more robust test which provides the most accurate result. You can sort of consider it the “gold standard” in sleep testing.
We take time to unplug me from the system and you are free to go home.
Someone will be monitoring your sleep the entire night and when you wake up we will unplug, answer any questions you may have and you will be on your way.
Most of the costs are covered by insurance plans.
CPAP
Answering this question is very difficult because it depends on each patient’s situation.
Some people are naturally born with smaller airways. This body “architecture” is determined by genetics and cannot be changed. In these patients, it can be assumed that the use of a CPAP should be done all throughout their life, unless surgery is possible.
At the back of the throat, there is an area called the Waldeyer ring. This region is composed of the palatine tonsils, lingual tonsils and adenoids. These organs function is to fight against infections. For various reasons, some patients’ tonsils are larger than normal (hypertrophic) and obstruct the airways. Their surgical removal can help reduce the severity of sleep apnea, but in most cases, it is not a very effective treatment.
Obesity
Obese patients represent the majority of CPAP users. Excess fat in the neck narrows the airway, causing sleep apnea. Significant weight loss could allow some patients to get rid of their CPAP. If you lose enough weight, a new sleep study could confirm that your apnea is gone and that you do not need CPAP anymore.
Alternative treatments
Patient adherence to CPAP is sometimes lacking. Some people cannot bear the idea of having a CPAP their whole life. In these cases, they should discuss alternative treatments for sleep apnea with a sleep professional. Today there is a variety of surgical and non-surgical alternatives to CPAP.
Sleep apnea treatment by continuous positive pressure, commonly known as CPAP (Continuous Positive Air Pressure) remains the most recognized treatment in the scientific literature. However, these results are directly dependent on the use of the device for a minimum of 4 hours per night. Some patients, after testing several types of masks, stop using their device because they fail to adapt. It is estimated that nearly 30% of users are intolerant to CPAP. In these patients, sleep apnea is not treated properly.
CPAP intolerance can create a sense of confusion. Fortunately, there are other ways to treat sleep apnea.
First, mandibular advancement devices (MAD) are dental devices that can treat patients with moderate apnea. See our page on these devices for more details.
Surgical solutions depend on the severity of the patient’s apnea. However, improving your lifestyle is required before considering any surgery. For example, being overweight compromises the success of different surgeries, therefore weight loss is necessary, especially in the case of CPAP intolerance. For mild apnea, minor palatal, lingual or nose surgeries can be performed with good success rates. Patients with severe apnea will benefit from orthognathic surgery. You should know that some treatments are covered by the Quebec health insurance while others are not.
If you suffer from a CPAP intolerance, our professional team can examine you to determine the possible treatments . You will then be better able to decide which one suits you.
You may decide not to wear your CPAP for one night for the following reasons: a cold with nasal congestion, night spent away from home, power failure, etc.
Some treatments, prescription glasses for example, only work when used. In the case of continuous positive airway pressure therapy with a CPAP device, it is not as simple.
CPAP, when used regularly, allows opening of the airways and counteracting against snoring and apnea. Over time, it helps reduce the inflammation caused by OSA. Since the volume of tissue is reduced, airways open easily and thus facilitate breathing. OSA symptoms may therefore take some time to resume.
Some patients fear that stopping their CPAP temporarily put their health at risk. They remember the risk of sudden death, stroke, or other heart problems their doctor told them about. You should know that the risk of these events happening after not using your CPAP for one night is infinitely small. Sleep apnea should be seen as a long-term risk factor. It can be compared to smoking: one cigarette will probably have no significant effect in the short term, but if you continue smoking for 30 years it will definitely damage your health.
You should not worry if ever something unexpected happens and your CPAP stays home and you have to sleep elsewhere. If your trip is planned, you can try bringing your CPAP with you to keep up your good habit. Otherwise, restart the treatment as soon as possible in order to continue benefiting from these effects on your long term health.
This is indeed an excellent question. What are the health effects of an untreated mild sleep apnea?
Consider the sleep apnea syndrome as being mild when the apnea – hypoapnea index (AHI) is between 5 and 15 events per hour. In 2006, the American Academy of Sleep Medicine (AASM) published a literature review with recommendations on the use of CPAP for treating sleep apnea. The review concluded that the scientific data were insufficient to recommend a systematic use of a CPAP for mild sleep apnea treatment.
One study compared changes in blood pressure following the treatment of mild sleep apnea syndrome and showed no difference compared to placebo. The impact of a CPAP in preventing cardiovascular risk in these patients remains unclear, possibly not significant.
A medical or conservative treatment is often recommended for a mild sleep apnea diagnosis. Such measures may include weight loss, positional therapy or the use of intranasal corticosteroids. Alternatives may also be considered before a CPAP such as the use of a mandibular advancement device which is effective in most cases of mild to moderate apnea.
Overall, the CPAP is not very beneficial for improving sleep apnea symptoms, such as daytime fatigue, cardiovascular risk and life quality in patients with mild sleep apnea. Not wearing your CPAP from time to time should not affect your long term health. A follow up with your doctor or specialist is recommended to ensure that your apnea remains stable over the years.
RAMQ does not cover any party of the CPAP machine. Payment typically is helped by a “health spending account” from private insurance companies.
Oral appliances
An oral appliance is $2500 – $3000 and is typically covered by insurance. The price range varies due to the different models and manufacturers.
Oral Appliances are well suited for people with mild to moderate sleep apnea, so in many cases patients have both. The gold standard for treating sleep apnea is a CPAP, however and it is required for those with severe apnea.
Surgery
The answer to this question is divided in two parts.
The first part that must be considered is whether your problem is snoring only or if snoring is combined with sleep apnea symptoms. While snoring is a problem affecting the lives of snorers and their entourage, corrective surgeries are generally considered “aesthetic” by the Régie d’Assurance Maladie du Québec (Quebec Medicare system).
In the case of a sleep apnea corrective surgery, you should know that all surgeries are covered by the RAMQ.
As far as prices are concerned, there are multiple possible surgeries and each case is unique. Our policy is to not give a price without having accurately assessed your situation. A sleep study is also required in all cases of snoring and sleep apnea. This study can be conducted in hospitals or in a private sleep laboratory.
In sleep apnea, airway obstruction can occur at different levels. The space behind the base of the tongue (oropharynx) is frequently involved. However, the space behind the soft palate (velopharynx) and the throat (hypopharynx) are often involved too. Orthognathic surgery by maxillary advancement will space out and increase the volume of these three areas. This intervention allows the advancement of the soft palate, the base of the tongue and the suprahyoid muscles without affecting them directly since it is jaws, to which theses structures are attached, that are moved.
The scientific journal SLEEP has recently published a literature review in which they analyzed nine studies on maxillary advancement surgery. These studies included a total of 234 patients with severe obstructive sleep apnea. After orthognathic surgery, they observed a 87% reduction of the overall AHI. This reduction allowed 232 of the 234 patients to completely correct their sleep apnea or at least lower it to a moderate level which, in both cases, symptoms were alleviated and CPAP wear was no longer required.
These results are not exclusive to this review. Several other recent studies have shown excellent success rates with this type of treatment. This suggests that orthognathic surgery is usually very effective in treating obstructive sleep apnea.
To find out if you are a good candidate for orthognathic surgery, please consult one of our professionals who can make an accurate assessment of your case.
Although patients with mild sleep apnea may see their condition improved after palatal surgery, it is not recommended by the American Academy of Sleep Medicine. A scientific literature review has identified a total of eight studies on the use of palate surgery to treat sleep apnea. The average apnea reduction was deceptive in most studies. Two of them recorded a worsening of symptoms.
Sleep apnea treatment first and foremost requires a sleep assessment by polysomnographic. This allows the sleep professional to confirm the diagnosis and assess the severity of the problem. Depending on the clinical examination, the professional may suggest different solutions. Non-surgical treatments are usually tried first, because of their conservative nature. If they are ineffective, sleep apnea correction by surgery may be offered.
Palate surgeries generally attempt to rebuild or strengthen the mobile portion of the soft palate. This part of the palate collapses during sleep and vibrates with air passage, therefore causing the snoring. Palate surgeries aim to correct this problem.
To know more about this, we invite you to visit our page on palate surgeries. You will find information about different types of treatment.
The effect on appearance depends on the type of surgery and its purpose. If the surgery only involves one of the two jaw bones, a 5 mm advancement will have a significant effect on facial physiognomy.
In the case of sleep apnea treatment, orthognathic surgery simultaneously affects both jaws. If the relationship between the two jaws is adequate, apnea correction will generally require an advancement ranging from 10 to 12mm. With such advancement, we can see a noticeable effect on the physiognomy, but altogether it remains harmonious and any change will appear modest. You should also know if tissues are soft and large (thick lips and cheeks, round face, slightly overweight), changes are less obvious. When the required advancement is more than 12mm, it becomes difficult or impossible to move the jaw without causing significant changes in physiognomy. These can even become unesthetic.
If you have concerns about physiognomic changes, please discuss this with your surgeon. He will tell you more about the effects of surgery.